Implementation of a Technician Checking Program at an Academic Medical Center
by Sara J. McEnaney, PharmD, MBA
March 9, 2011
Implementation of a Technician Checking Program at an Academic Medical CenterAs published in KeePosted, Official Newsjournal of the Illinois Council of Health-System Pharmacists (Volume 37, Issue 02)
by Sara J. McEnaney, PharmD, MBA
Pharmacy Clinical Specialist, Regulatory Compliance, Internal Audit, Performance Improvement and Training
Rush University Medical Center
Background
Technician checking programs are gaining popularity in hospital pharmacies to allow pharmacists to focus their time on more clinical functions including answering drug information questions and providing medication-dosing recommendations. Wisconsin law states a pharmacist is responsible for the final check of medications. However, the Pharmacy Examining Board (Board) in the state of Wisconsin has granted variances to hospitals to allow pharmacy technicians to check unit dose cart fill. The purpose of this study was to design and implement a technician checking program and to assess the baseline checking accuracy of a pharmacist compared to that of a trained and validated technician.
Froedtert Hospital (FH) is a 500-bed academic medical center located in Milwaukee, Wisconsin. FH pharmacy department is continually looking for ways to optimize the medication distribution model. The goal for medication distribution is to have a seamless system from receipt of medication from the wholesaler to administration to the patient with barcode verification at every step of the process. The unit dose drug distribution model used at FH is documented in Figure 1.
Figure 1 Unit dose drug distribution model used at Froedtert Hospital
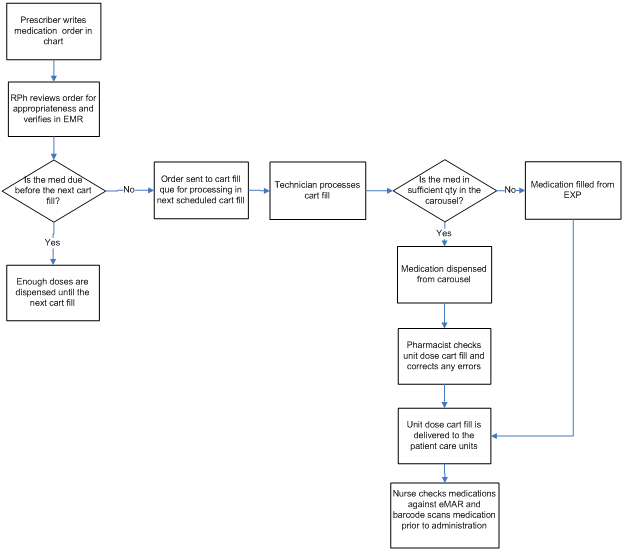
Pharmacists working in the central pharmacy are responsible for all clinical monitoring for assigned patient care units. Pharmacists evaluate all medication orders for appropriateness prior to verification in the electronic medical record (EMR). Upon verification, any medication doses needed prior to the next scheduled cart fill are dispensed from the central pharmacy.
The twenty four hour cart fill is downloaded through the EMR and sent to the medication carousel and high speed repackaging machine for processing. The technician removes medications from the carousel and puts them into patient specific medication drawers. A pharmacist is responsible for performing the final check of these medications, an important but time-consuming task that limits the amount of time spent on clinical activities. Nurses are also responsible for checking medications against the electronic medication administration record and barcode scanning the patient’s armband and the medication prior to administration to the patient.
A technician checking program allows specialty trained technicians to perform the final check on certain medications filled by another technician. Pharmacy literature has demonstrated these programs are as safe and effective as having a pharmacist perform the final check1-2. By using pharmacy technicians to take on more responsibility for distributive tasks, this allows pharmacists to spend time on clinical activities.
Methods
This study was designed in a similar fashion to a previous study conducted by Ambrose et al1. The first phase of the study was to develop a technician training program, present the program to the Board and validate technicians who successfully complete all steps of the program. The second phase of the study was to assess the baseline accuracy of pharmacists checking the unit dose cart fill and ADC refills. The third phase was to evaluate accuracy of technicians checking the unit dose cart fill and ADC refills. The fourth and final phase is to develop quality assurance audits for the technician checking program and to maintain data to present to the Board.
Phase one involved the creation of a technician checking program deemed acceptable by the Board. Minimum requirements to participate were defined by the hospital. To participate in the program a technician must be working full time with at least one year of technician experience and be a Certified Pharmacy Technician (CPhT) through the Pharmacy Technician Certification Board (PTCB). The training program consisted of two parts: A self-learning packet and a simulated checking environment. The self-learning packet contained several sections including: Introduction to the technician checking program, qualifications / validation / quality assurance (QA), elements of packaging and product characteristics, medication errors and the medication distribution process. A pharmacist reviewed the sections of the self-learning packet with the technician explaining details and requirements of the program. The technician was then given a week to review the self-learning packet and answer the self-assessment questions. Any incorrect answers would be discussed with the technician. The technician was required to score 90% on the test questions to move on to the next phase of training the simulated checking environment.
The simulated checking environment was developed to mirror the unit dose cart fill. Intentional errors were introduced throughout the simulated environment prior to the technician checking. The technician checked the entire simulated cart and documented any errors identified. Upon completion, the technician discussed all errors identified with the auditing pharmacist. The technician was required to score 90% prior to entering the final phase of training the validation period.
During the validation period the technician was required to maintain a 99.8% accuracy rate in checking at least 3,500 consecutive doses, during at least five separate audits. The audit process consisted of a registered pharmacist checking the accuracy of unit dose cart fill drawers or ADC refills after the technician checked them. Any errors resulting from improper checking were documented and recorded on the validation log. The pharmacist auditor discussed the errors with the technician as they were encountered. During the validation process the technician filling the carts intentionally introduced errors at a minimum rate of 0.2% (seven doses per 3,500). The pharmacist auditor had a record of the intentional errors to ensure they were removed prior to distribution of medications to the patient care areas. Intentionally introduced errors included an occurrence of a wrong drug, a wrong dose, a wrong dosage form, an extra or insufficient quantity and an omitted medication. The pharmacist auditor evaluated the technician checker using the Validation Competency Assessment Checklist (see Figure 2). If a technician missed more than seven errors per 3,500 doses, they failed the validation. If a technician did not achieve the required 99.8% accuracy level in checking 3,500 consecutive doses after two months of training, the technician was no longer eligible to participate in the technician checking program. Upon successful completion of the validation (99.8% accuracy rate) the technician was recognized as a Validated Technician Checker (VTC).
Figure 2 Validation Competency Assessment Checklist
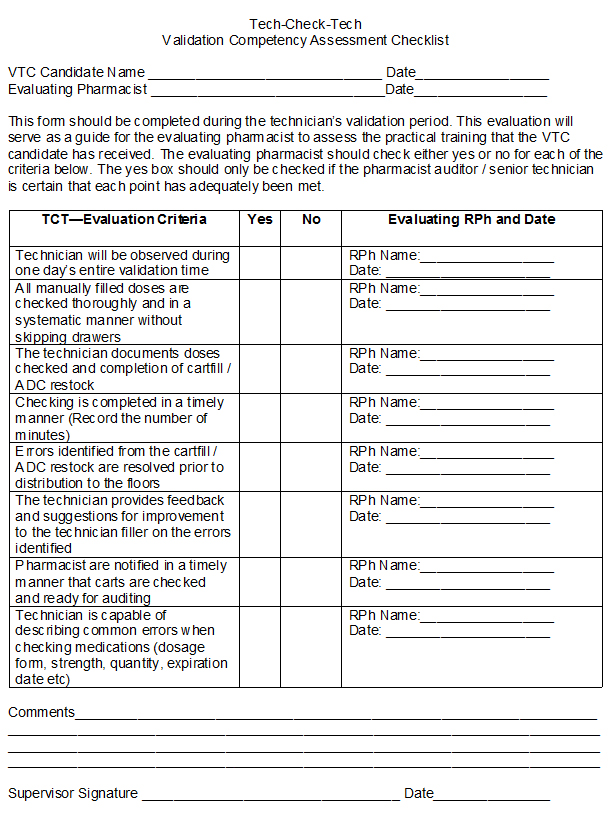
The technician checking program was presented at the Board Meeting in December 2009 and a variance was granted until March 2011. FH is required to submit technician specific QA data to the Board at six month intervals for the duration of the variance.
Phase two began in October 2009 upon completion of training and validation of selected technicians. The goals of this phase were to audit 3,500 cart fill doses and 2,000 ADC refill doses. All participants were aware that audits were being conducted on checking accuracy. Third shift pharmacy technicians filled the carts according to their normal workflow. The technician filling the carts documented and introduced intentional errors at a rate of seven errors per 3,500 doses to correspond to a 99.8% minimum accuracy rate required by the Board. The pharmacist checking the cart fill or ADC refills documented and worked with the filling technician to correct all errors that were detected. A pharmacist auditor then rechecked all medications to verify the accuracy of a pharmacist checking cart fill and ADC refills. Any errors overlooked by the checking pharmacist were documented and corrected before medications were delivered to the patient care units.
Phase three began immediately upon the completion of phase two with the same goals. Participants were again aware that audits were being conducted for checking accuracy. Phase three followed the same procedures as phase two, however, a technician was doing the initial check followed by a pharmacist auditor.
Phase four, the QA program, is ongoing as the technician checking program is being implemented. For the QA program, a pharmacist is required to check ten percent of all doses checked by a VTC. The results of this check are documented in the QA database and maintained on site and submitted to the Board at six month intervals. As part of the QA program, ongoing standards for technician participation were implemented to maintain safety and accuracy for medication distribution. If the accuracy of the VTC is less than 99.8% over the lesser of a six month period or for the first 2,000 double checked doses within a six month period, the VTC is required to be re-trained and re-validated (3,500 doses, 99.8% accuracy). If the accuracy of the VTC is less than 99.8% on more than four occasions in a year, the VTC will be relieved from their VTC status for a six month period. The technician checker may be re-trained and re-validated after the six month period. If the re-validated technician checker has less than 99.8% accuracy on any occasion during the three months following their six-month leave, they will be permanently removed from their VTC status and unable to participate in the technician checking program. If a VTC does not check for more than two months, re-validation (99.8% accurate, 3,500 doses) should be done with the first check upon return. If the VTC does not check for four months, they must be re-trained and re-validated.
Results
Four pharmacists participated in phase two of the study to assess the baseline accuracy of a pharmacist checking the unit dose carts and ADC refills. Three technicians successfully completed the training requirements and were validated to participate in phase three of the study. Table 1 displays the results from phase two and three of the study. The mean accuracy rate for pharmacists checking the cart fill was 99.93% and 99.85% for technicians (p=0.054). The mean accuracy rate for pharmacists checking the ADC refills was 99.40% and 100% for technicians (p<0.001). The difference in accuracy rates for pharmacists and technicians was not significant for cart fill, but was significant for ADC refills. The mean accuracy rate for technicians for unit dose cart fill and ADC refills was higher than the 99.8% required by the Board. After three months of the program, all VTC had maintained a minimum accuracy rate of 99.8% during the required 10% percent audits and no technicians had been required to complete any of the ongoing standards for failed QA audits. Technician specific QA data will be presented to the Board at six-month intervals (see Table 2).
Table 1 Results from phases two and three of the study
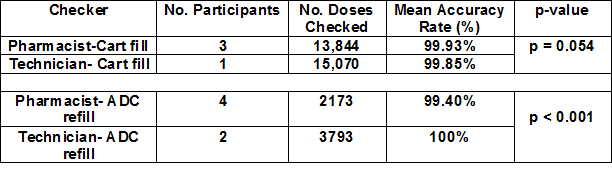
Table 2 Technician specific QA data
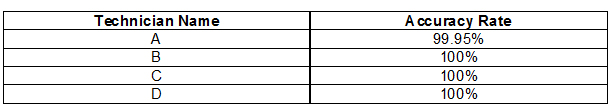
Discussion
The results of this study support the hypothesis that well trained technicians can accurately check unit dose cart fill medications filled by another technician. This is similar to what has been published in the literature1-2. The study also demonstrated that technicians could maintain at least a 99.8% accuracy rate when checking ADC refills.
It was determined that pharmacists spend approximately two hours on third shift checking the unit dose cart fill. Throughout the day pharmacists also spend approximately one to two hours checking the ADC refills. With the implementation of the technician checking program, pharmacists are required to check ten percent of these doses requiring approximately thirty minutes total each day. The time saved by the pharmacists is now spent on clinical activities within the central pharmacy for the assigned patient care areas. The senior pharmacy technician for operations is responsible for training and coordinating the validation of technicians for continued expansion of the technician checking program.
Some limitations to this study have been identified. The pharmacists and technicians who participated in the study were not randomized. The technicians were selected based on meeting baseline requirements for participation in the program and availability during the study period. The pharmacists volunteered to participate in the study based on schedule availability. The pharmacists and technicians were all aware that accuracy studies were being conducted. Also, the intentional errors in the study were not randomly introduced. The technicians filling the cart or ADC refill would introduce errors as required by the study guidelines. However despite these limitations, the QA program implemented has shown that technicians are able to maintain the minimum accuracy rate required for continued participation in the program. VTC have been given increased responsibilities in the central pharmacy which has contributed to overall job satisfaction.
Conclusion
This study demonstrated that technicians could accurately check ADC refills. This study also reaffirmed previous literature stating pharmacy technicians who have been adequately trained and validated through a technician training program can accurately check unit dose cart fills while maintaining patient safety in medication delivery. Â?"
References
1. Ambrose PJ, Saya FG, Lovett LT, et al. Evaluating the accuracy of technicians and pharmacists in checking unit dose medication cassettes. Am J Health-Syst Pharm. 2002; 59:1183-8.
2. Woller TW, Stuart J, Vrabel R, Senst B. Checking of unit dose cassettes by pharmacy technicians at three Minnesota hospitals. Am J Hosp Pharm. 1991; 48:1952-6.
